RHT Program 2026: A Roadmap for Rural Healthcare Transformation

Access to quality care should not be determined by a zip code. Yet, as of 2025, nearly 60 million Americans living in rural communities continue to face a higher risk of death from preventable causes compared to their urban counterparts.
To address these systemic gaps, the Centers for Medicare & Medicaid Services (CMS) introduced the Rural Health Transformation (RHT) Program, authorized by the One Big Beautiful Bill Act (Public Law 199-21).
In December 2025, all 50 states received awards under this initiative, which is specifically designed to support rural primary care providers, including Federally Qualified Health Centers (FQHCs), Rural Health Clinics (RHCs), and small independent practices that serve as the backbone of their communities.
The RHT Program is not just a standard grant. It is a strategic shift toward a value-based model that prioritizes whole-person care. For FQHCs or rural practices, this means receiving the support needed to integrate primary care with behavioral health and social services.
As we look toward the 2026 implementation, understanding the eligibility requirements, technology standards, and performance expectations is critical for success.
Explore our FQHC Solutions
What is the Rural Health Transformation Program?
The RHT Program provides $50 billion in total funding over five years (FY 2026-2030) to address the financial and clinical challenges inherent in rural health. In December 2025, all 50 states received awards to implement state-led transformation initiatives.
The program is built on five strategic goals: making rural America healthy again, ensuring sustainable access, workforce development, innovative care models, and tech innovation. Half of this funding is distributed evenly among approved states as baseline funding.
The remaining $25 billion is workload-driven, awarded based on specific rural factors, the quality of state applications, and the clinical initiatives they propose. This structure ensures that states with the greatest need and most comprehensive plans receive proportional support.
Who is This Program For?
While the program is managed at the state level, actual care delivery occurs through rural providers who receive subawards and grants from their state. CMS has designed the RHT Program to be inclusive of various rural provider types. Eligible recipients of state funding include:
- Federally Qualified Health Centers (FQHCs):
Community-based providers that receive funds from the HRSA Health Center Program to provide primary care services in underserved areas. - Rural Health Clinics (RHCs):
Clinics located in rural, underserved areas that are certified to receive special Medicare and Medicaid reimbursement. - Small Rural Primary Care Practices:
Independent or small group practices that provide essential care to rural populations. - Tribal Health Programs:
Health programs operated by Indian Tribes or Tribal organizations.
By focusing on these specific entities, the RHT Program ensures that the most critical access points in the rural health ecosystem receive the resources they need.
How Will Funding Be Distributed?
Understanding the flow of RHT funding is vital for strategic planning. Each state designated a lead agency (typically the State Medicaid Agency or Department of Health) to administer the program within its state.
This state agency is responsible for distributing funds to rural providers such as your FQHC or RHC through competitive grants, requests for proposals (RFPs), and contracts. The funding supports two main areas. First, states receive administrative funding to build the infrastructure needed to manage the program.
Second, states provide direct grants and payments to rural providers to support activities such as upgrading medical software, expanding telehealth technology, and improving revenue cycle management. This structure ensures that practices remain financially viable as they transition to new care delivery models.
How to Apply for RHT Program Funding
The RHT Program has two phases. After state applications closed in November 2025, awards were announced to all 50 states in December. States are now preparing funding opportunities for rural FQHCs and clinics, which must apply directly to their state's RHT program.
Most states will release application details and funding opportunities in Spring and Summer 2026. If your clinic is in a rural area, contact your State Medicaid Agency or Department of Health for information on eligibility and timelines.
Before applications open, evaluate your technology capabilities, such as EHR data exchange and telehealth infrastructure, as these will influence your competitiveness for funding.
Interoperability and Telehealth Solutions
Eligible Uses and Approved Activities
The RHT Program encourages investment in areas that directly impact patient outcomes and practice efficiency. CMS specifically highlights the need for better service integration. Eligible uses for the funding typically include:
- Telehealth Expansion:
Improving telehealth in rural areas to reach patients who face transportation or mobility barriers. - Data Analytics:
Utilizing AI for healthcare to identify high-risk patient populations and intervene before chronic conditions worsen. - Infrastructure Upgrades:
Implementing robust medical software that supports interoperability and detailed clinical reporting. - Care Coordination:
Strengthening the link between primary care and behavioral health solutions to treat the whole patient.
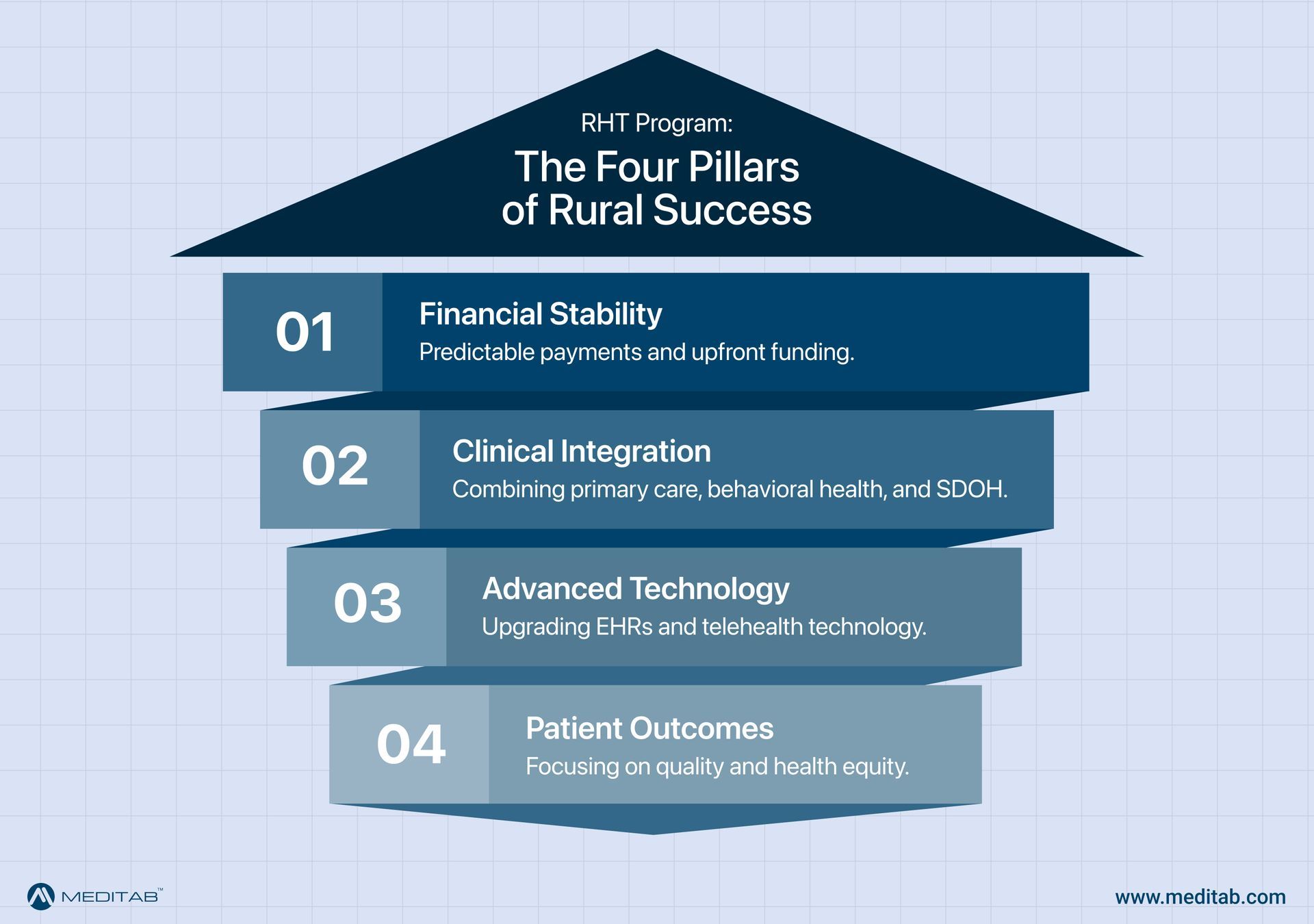
Technology Requirements That Matter for RHT Success
The success of any healthcare transformation depends heavily on the tools providers use. For rural FQHCs and clinics, a basic electronic record system is no longer sufficient to meet the demands of value-based care. To succeed in the RHT Program, practices need a partner that offers:
- Seamless Integration:
Your EHR must integrate primary care with behavioral health and social determinants of health (SDOH) tracking in a single interface. - Advanced Revenue Management:
As payment models shift, your revenue cycle management must be agile enough to handle complex, non-traditional contracts. - Scalable Telehealth:
You need telehealth technology that works reliably, even in areas with lower internet bandwidth, to ensure constant patient access.
Meditab has spent decades perfecting the
IMS to meet the specific needs of rural clinics and FQHCs, ensuring that these providers have access to the same high-level tools as large urban networks.
A New Opportunity for Rural Health Providers
The RHT Program represents a turning point for the American healthcare system. It acknowledges that rural health cannot be fixed with a one-size-fits-all approach. By providing the capital and the framework to innovate, CMS is giving FQHCs and small practices the power to redefine what care looks like in their communities. While the administrative shift may seem complex, the potential for improved patient health and long-term practice stability is unprecedented.
Conclusion
The Rural Health Transformation Program is more than a funding opportunity. It is a blueprint for the future of rural health care. For FQHCs and rural clinics, 2026 is the time to evaluate internal workflows, strengthen state-level partnerships, and invest in the health solutions that will drive success. By staying informed and proactive, your practice can lead the charge in this essential transformation.
Book a Software Discovery
Frequently Asked Questions
How does the RHT Program help with EHR implementation?
The program provides participant payments to upgrade medical software and infrastructure, ensuring practices can meet new data and reporting requirements.
What does "multi-payer model" mean for my clinic?
It means the Lead Entity works to align Medicare, Medicaid, and private insurers within a single value-based payment and care delivery framework to ensure consistency for providers.
Is the RHT Program only for FQHCs?
No. While FQHCs are a primary focus, the program is also open to Rural Health Clinics (RHCs), small rural primary care practices, and Tribal health programs.
When should my practice start engaging with the RHT Program?
Immediately. States are developing their implementation plans and RFPs. Practices should contact their State Department of Health or Medicaid Agency to learn about upcoming funding opportunities and ensure they are positioned to apply when applications open.
What technology standards must my EHR meet to qualify for RHT funding??
Your EHR must support FHIR standards for interoperability, comply with USCDI data elements, participate in Health Information Exchanges, and meet 21st Century Cures Act requirements for information access. Systems that cannot demonstrate these capabilities may require upgrades before you can fully participate in the program.












