Key Strategies for Optimal Revenue Cycle Management

A healthcare practice operates on a delicate balance. While the primary focus remains on patient outcomes, the clinic's administrative and financial health dictates its ability to continue providing that care.
Over 30% of U.S. healthcare organizations are piloting or planning autonomous coding solutions, signaling how critical automation has become to reducing errors and accelerating reimbursements. This is where revenue cycle management becomes the most critical asset for any provider.
In its simplest form, the revenue cycle encompasses every step from the moment a patient schedules an appointment to their final payment. However, as regulations shift and insurance requirements become more complex, managing this cycle effectively requires more than just submitting claims.
It requires a strategic, end-to-end approach that integrates technology, staff expertise, and data-driven insights.
Improve Your RCM Today
What is Revenue Cycle Management?
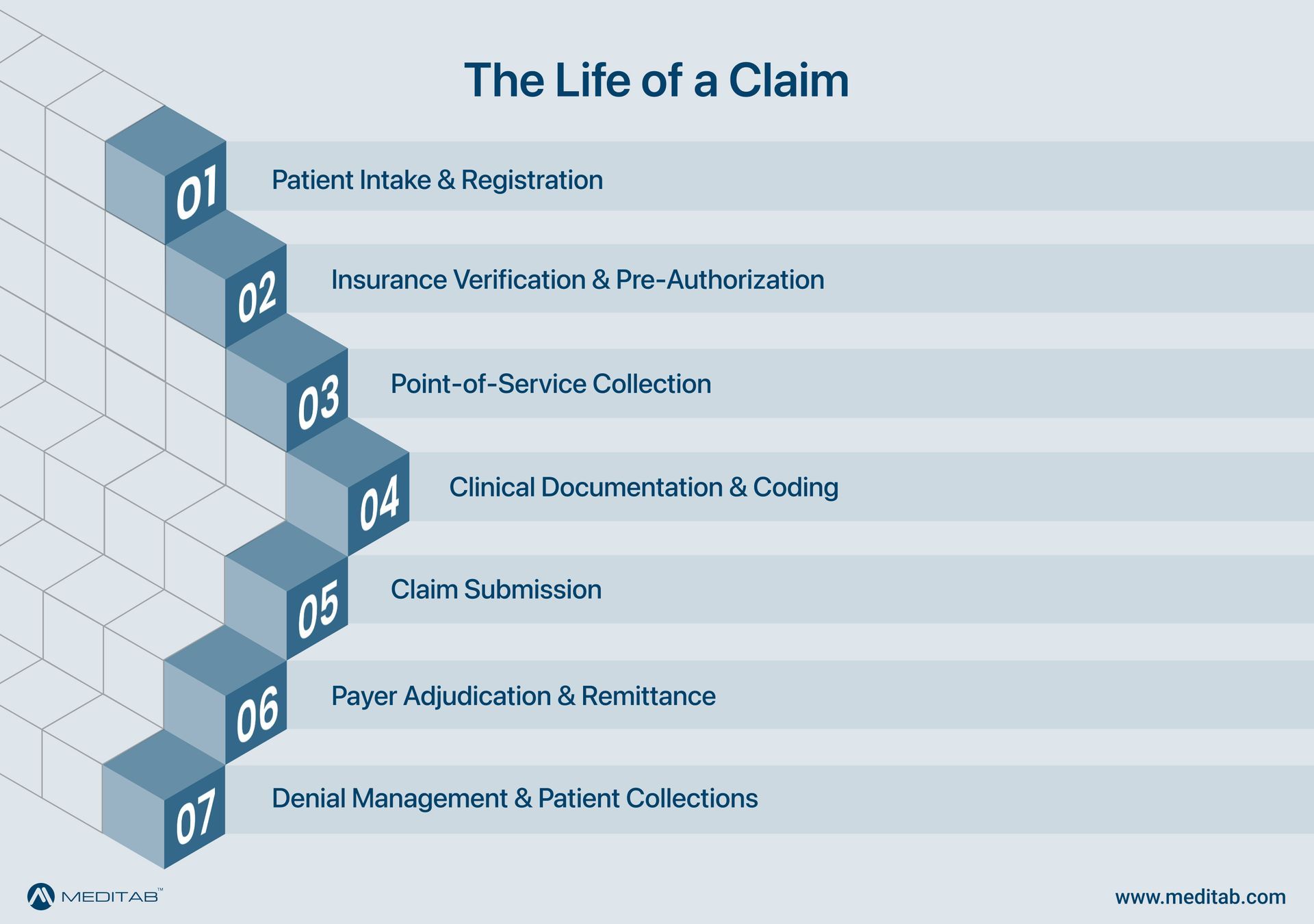
In the healthcare domain, RCM in medical billing refers to the strategic process facilities use to track patient care episodes from registration and appointment scheduling through final payment of a balance. It involves several moving parts: verifying insurance, capturing charges, coding, submitting claims, and managing collections.
When these steps are disconnected, errors occur. A small mistake during patient intake can lead to a claim denial weeks later. This is why many organizations are relying on specialized RCM services or integrated RCM software to ensure nothing falls through the cracks.
Why Revenue Cycle Management Matters
The aim of any medical revenue cycle management plan is to ensure that the practice is reimbursed for its services as soon as possible. Poorly managed RCM leads to high denial rates, wasted administrative time, and cash flow disruptions.
Effective healthcare RCM also improves the patient experience. Transparent billing helps improve patient satisfaction. It reduces frustration and increases trust. With improved workflow, you can help your clinical staff focus more on patients and less on administrative headaches.
1. Prioritize Front-End Accuracy
The revenue cycle begins long before any direct interaction with the patient. Accuracy begins at the front desk, and for revenue cycle management services to succeed, you need to make sure your staff is diligent about ensuring they check for patient insurance coverage and authorizations before they come in for services. Incorrect patient identification and/or policy number are among the top reasons for claim denials.
2. Leverage Comprehensive RCM Software
Manual tracking can lead to significant errors. Improve this process by transitioning from spreadsheets and disparate systems to
integrated RCM software that connects your EHR directly to billing. This automation enhances charge capture and claim submission, eliminating manual data entry and providing real-time checks that identify issues, such as missing information, before claims are submitted. Implementing automation can decrease administrative costs per claim by
nearly 25%.
3. Focus on Denial Management
Many practices view denied claims as lost causes or delay appeals for too long. Shift from reactive appeals to proactive analysis by replacing manual denial logs with software dashboards that track coding errors weekly. Implement staff training on these patterns to prevent recurrences. This can
eliminate up to 85% of avoidable denials, reducing rates from around 12% to under 5%.
4. Simplify Patient Payments
As patient out-of-pocket costs rise, collecting from individuals has become more challenging than collecting from payers. To help with this, medical billing services for small practices often recommend offering multiple payment avenues. Online portals, text-to-pay options, and clear cost estimates before treatment can significantly improve your collection rates.
5. Regular Staff Training
The landscape of medical coding and payer policies is constantly shifting. Regular training for your billing and coding staff is essential to stay compliant and efficient. Even the best RCM tools require a team that understands the industry's nuances.
Conclusion
Effective revenue cycle management is the backbone of a sustainable healthcare practice. By focusing on front-end accuracy, utilizing the right technology, and staying proactive with denial management, you can protect your practice from financial instability.
Remember, a streamlined billing process doesn't just help your bank account; it creates a more professional, stress-free environment for both your staff and your patients. If managing these complexities in-house feels overwhelming, exploring professional RCM services might be the right step toward ensuring your practice continues to thrive for years to come.
Medical Billing Simplified
Frequently Asked Questions
What is the most common cause of claim denials?
The majority of denials stem from front-end errors, such as incorrect patient information or failure to verify insurance eligibility. Coding errors and a lack of prior authorization are also frequent culprits.
How does RCM software improve practice efficiency?
RCM software automates repetitive tasks like claim scrubbing and status tracking. This reduces the likelihood of human error and allows your billing team to focus on resolving more complex issues.
Should small practices outsource their RCM?
Many find that medical billing services for small practices provide a high return on investment. Outsourcing can provide access to expert billers and advanced technology without the overhead costs of a full in-house department.
How often should we audit our revenue cycle?
It is good practice to perform a deep-dive audit at least once, and twice a year, though monitoring key performance indicators (KPIs) like your net collection rate should happen monthly.












