The Ultimate EHR Implementation Guide for Ambulatory Practices

The global
ambulatory EHR market size was estimated at USD 9.47 billion in 2025. This growth has been steadily rising, and reports suggest that it will grow from USD 9.94 billion in 2026 to USD 15.93 billion by 2034. Despite the constant rise in market share, the dilemma for ambulatory practices remains: whether to invest in a trusted Electronic Health Record (EHR) system. A well-planned EHR implementation can transform daily operations, improve patient care, and strengthen financial performance. Done incorrectly, however, it can disrupt workflows, frustrate staff, and create costly setbacks.
When it comes to independent practices, specialty clinics, and growing outpatient groups, having a clear EHR implementation plan is essential. This guide walks you through the complete EHR implementation process for IMS (Intelligent Medical Software), from early preparation through successful go-live to long-term optimization.
What is an EHR?
An Electronic Health Record (EHR) is a digital, real-time version of a patient’s complete health history, designed to go beyond the standard clinical data collected in a single provider's office. It provides a patient-centered record that makes information available to authorized users instantly and securely across the care continuum. The growth in this sector is expected to be at a
CAGR of 5.73% over the forecast period 2024-2032.
What Is EHR Implementation?
EHR implementation is the full process of selecting, preparing for, installing, and adopting a new EHR system in your practice. It covers everything from planning and data migration to staff training, testing, and ongoing optimization.
A successful EHR system implementation ensures the software is not only installed but also fully embraced by your entire team. Implementation of
EHRs supports disease and quality management. In one study, 80% of interviewed physicians reported a positive effect of systematic information storage in EHRs on disease management.
The Importance of a Successful EHR Implementation
A successful EHR system implementation is the bedrock of a modern practice. When executed correctly, it does more than just replace paper; it enhances the accuracy of clinical documentation, improves patient safety through real-time alerts, and optimizes the revenue cycle.
For outpatient clinics, the stakes are high. A flawed implementation can lead to provider burnout, patient frustration, and significant financial leakage. Conversely, a successful launch ensures that your EHR functionalities actually serve your staff, allowing them to spend less time on screens and more time on patient care.
According to the 2022 National Hospital Ambulatory Medical Care Survey (NHAMCS), ambulatory centers in the U.S. recorded over 155 million patient visits in 2022. Managing this high patient load requires scalable EHR solutions to handle data collection, scheduling, and clinical documentation effectively. As visit volumes grow, providers are increasingly dependent on EHR systems to maintain smooth operations and ensure accurate patient records, which directly drives market expansion.
Understanding the EHR Implementation Process
The EHR implementation process typically follows a structured sequence of phases. While every practice is unique, most successful implementations include planning, configuration, training, testing, go-live, and post-implementation support. Learn more about Meditab’s IMS Implementation Process.
Preparing for EHR Implementation
Preparation is where the success of your EHR implementation journey is decided. Per the Office of the National Coordinator for Health Information Technology, in 2023, nearly 93% of U.S. office-based physicians had implemented an EHR system, with 85% using certified ones. Before any software is installed, the practice must lay the groundwork:
- Assemble Your EHR Selection Team: Include clinicians, administrative staff, and billing leads. This ensures that the chosen system supports both clinical and financial workflows.
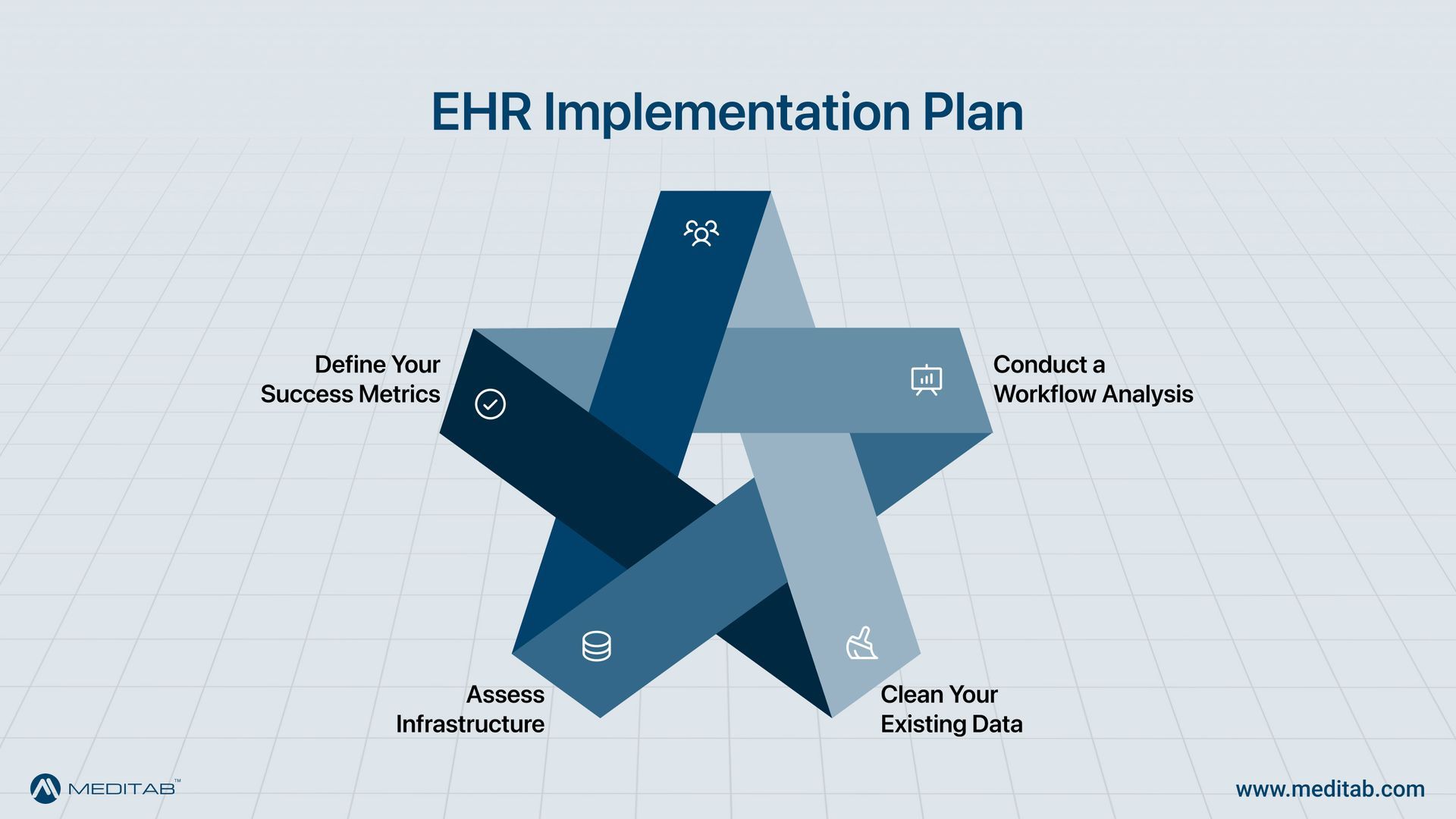
- Conduct a Workflow Analysis: Document current "paper-based" or legacy digital paths to identify where the new system can automate tasks or where old habits might hinder digital progress.
- Clean Your Existing Data: Before migrating anything, audit your current patient data. Remove duplicates, standardize formats, and verify critical information. Dirty data transferred into a clean new system creates ongoing problems.
- Assess Infrastructure: Ensure your hardware, internet bandwidth, and mobile devices are compatible with modern ambulatory systems.
- Define Your Success Metrics: What does a successful EHR implementation look like for your practice? Common metrics include:
- Reduced documentation time per patient
- Increased first-pass claim acceptance rate
- Faster patient check-in times
- Higher staff satisfaction scores
How Long Does EHR Implementation Take?
While North America dominated the ambulatory EHR market with a 47.26% market share in 2025, the successful adoption of these systems depends on tailored EHR implementation. The duration of this implementation varies according to practice size, specialty complexity, and specific customization needs. These specifics have been listed below:
- Small clinics: 2–4 months
- Mid-sized practices: 4–8 months
- Multi-specialty ambulatory groups: 6–12 months
Meditab exceeds these market standards by successfully delivering accelerated implementation timelines. For small practices, we can achieve a complete rollout in as little as 4 weeks, provided there is a mutual commitment to the timeline and prompt data delivery for conversion. Our general average across the board remains an efficient 6–8 weeks, largely due to the standard 6-week window required for Medicare billing registration.
For medium-sized clinics, our streamlined process typically concludes within 8–12 weeks, while larger, more complex organizations are generally fully operational within 12 weeks to 6 months, depending on the practice's specific requirements. By choosing Meditab, practices can reduce their transition period and begin realizing the benefits of their new EHR system weeks or even months ahead of the industry average.
EHR Implementation Steps and Process
The integration of patient portals within ambulatory EHR platforms is also contributing to market growth by improving patient engagement. According to the data published by the Assistant Secretary for Technology Policy, in 2021, 4 of 5 office-based physicians adopted an EHR system. A typical EHR implementation plan includes these key steps:
- Planning and Vendor Selection
Define requirements, evaluate options, and select the best-fit EHR vendor.
- Project Kickoff
Assemble your team and establish clear roles and communication.
- Clearinghouse Selection & Registration
Select and register with a Clearinghouse early in the process. This step significantly impacts your go-live plan, as credentialing and electronic data interchange (EDI) setups can take several weeks to finalize.
- Data Migration
Carefully transfer historical patient records from your old system.
- System Configuration
Customize templates, workflows, and integrations to match your practice.
- Staff Training
Provide comprehensive training for all users before go-live.
- Testing and Validation
Run thorough tests to ensure everything works as expected.
- Go-Live
Launch the new system, often in stages to reduce risk.
- Post-Go-Live Support
Monitor performance, address issues, and continue optimizing workflows.
Key Strategies for Implementation
Utilizing proven EHR implementation strategies can mitigate common risks:
- Start with "Why"
Before teaching "how," remind everyone why the practice is making this change, and connect the new EHR to reducing burnout, improving patient care, and driving practice growth.
- Phase Your Rollout
The large practices segment accounted for the largest share of the global ambulatory EHR market in 2021, at 47.4%. Therefore, for this sector, it is recommended that there be a phased EHR integration strategy approach:
- Go live with scheduling and demographics first.
- Add clinical documentation one week later.
- Bring billing live after clinical workflows stabilize.
- The "Super User" Model
Identify tech-savvy staff members to receive advanced training early. They act as the first line of on-site support for their peers during the transition.
- Use Sandbox Environments
Create a training environment where staff can practice without affecting real patient data. Allow unlimited "mistakes" in sandbox mode.
- EHR Integration Strategies
Your EHR shouldn't be an island. Prioritize EHR integration strategies that connect your records with labs, imaging centers, and pharmacies from day one to reduce manual data entry.
- Clear Communication
Keep all stakeholders informed. When staff understand the "why" behind the change, they are more likely to adopt the new system with a positive mindset.
- Celebrate Milestones
EHR implementation is hard work. Celebrate the completion of training, successful testing, and the go-live week. Recognition builds momentum.
EHR Implementation Challenges
Even with careful planning, practices often face challenges, including staff resistance, data migration issues, temporary productivity dips, and integration complexities. For more details on overcoming these hurdles, read our guide on
avoiding common EHR implementation challenges.
Optimizing Workflow and Maximizing the Benefits of EHR
Once the initial launch phase concludes, the focus shifts to optimization. Among the various deployment types, cloud-based EHR deployments lead with an over 58% share in 2024, driven by scalability, flexibility, and cost-effective healthcare IT solutions. High-performing practices regularly review their EHR functionality to identify underutilized tools. Optimization includes:
- Automating Patient Engagement: Using portals for self-scheduling and digital check-ins.
- Advanced Reporting: Leveraging data analytics to track clinical outcomes and financial health.
- Continuous EHR System Maintenance: Regularly updating the software to access new security patches and features, ensuring the system remains a long-term asset.
Choose the Best EHR System
Selecting the right partner is critical for a successful EHR system implementation. Meditab offers a robust, cloud-based ambulatory EHR designed to simplify clinical workflows, improve efficiency, and enhance patient engagement.
With a strong focus on usability and customization, we support practices throughout the entire EHR implementation journey from planning and configuration to training and optimization. Our proven implementation framework ensures smooth adoption, minimal disruption, and long-term success for ambulatory providers.
The Bottom Line
Primary care physicians’ EHR capability to identify patients for care reached up to
72.9% in terms of EHR adoption rate. A successful EHR implementation is about more than installing software. It’s about transforming how your practice delivers care. With careful planning, the right partner, and a focus on people and processes, your EHR implementation journey can deliver lasting improvements in efficiency, revenue, and patient outcomes.
Frequently Asked Questions (FAQs)
What is the typical timeline for EHR implementation?
It typically takes between 2 and 12 months, depending on practice size and complexity.
What are the key steps in EHR implementation?
The most critical EHR implementation steps are: assembling the right team, cleaning existing data, configuring specialty-specific templates, thorough staff training, running parallel tests, and having vendor support during go-live. Skipping any of these increases the risk of failure.
What is the most important part of an EHR implementation plan?
While every step matters, staff training and workflow analysis are the most critical. Without staff who know how to navigate the system, even the most advanced EHR functionalities will not be utilized to their full potential.
What are the biggest challenges during EHR implementation?
Common challenges include workflow disruption, resistance to change, and data migration issues.
What is the difference between cloud-based and on-premise EHR implementation?
Cloud-based (or remote-hosted) EHR system implementation involves the vendor managing servers and updates, requiring minimal internal IT. On-premise implementation requires purchasing hardware, installing software, and managing ongoing maintenance, which is now rare for most ambulatory practices.












