IMS: The All-in-One EHR, Practice Management, and Billing Software
Intelligent technology that adapts to your practice, not the other way around.
✓ Fully Customizable
✓ Tailor-Fit for 40+ Specialties
✓ Cloud and Mobile Capabilities
IMS: The All-in-One EHR, Practice Management and Billing Software
Intelligent technology that adapts to your practice, not the other way around.
✓ Fully Customizable
✓ Tailor-Fit for 40+ Specialties
✓ Cloud and Mobile Capabilities
Take the path to better your practice. Start
HERE!
Slide title
Write your caption hereButton
Slide title
Write your caption hereButton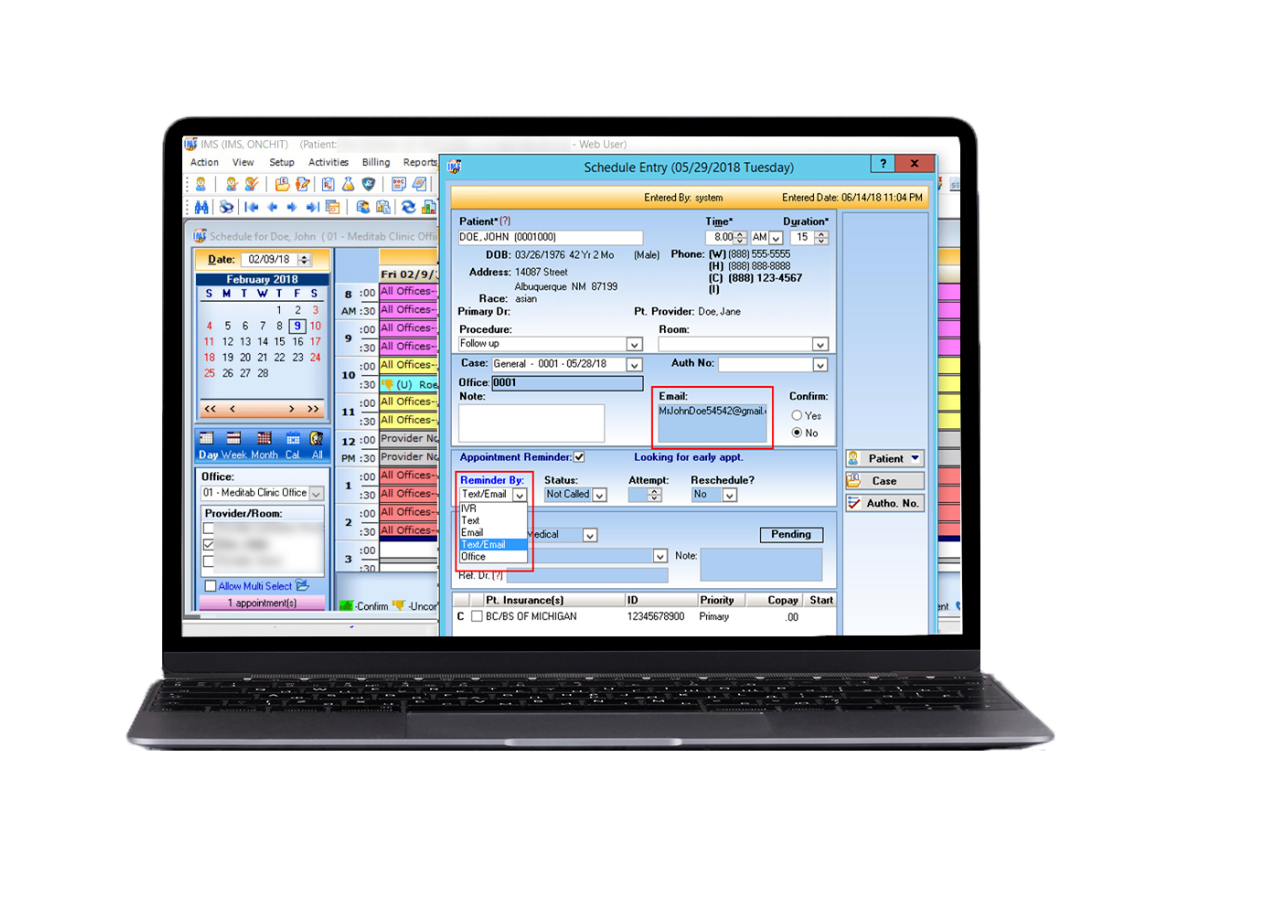
Slide title
Write your caption hereButton
Slide title
Write your caption hereButtonSlide title
Write your caption hereButton
-

EHR
Our EHR system is aligned to meet the demands of a broad and diverse network of healthcare providers.
Learn More → -

EMO
A new branch of modules that expands what IMS delivers for your practice, EMO is the efficiency you’ve always wanted. Whether it’s your front desk, back office, or waiting room, run your medical office like the fine-tuned business it is with our new medical software.
Learn More → -

Practice Management
Our comprehensive practice management tool can boost your medical staff's efficiency, medical billing processes, and patient flow.
Learn More → -

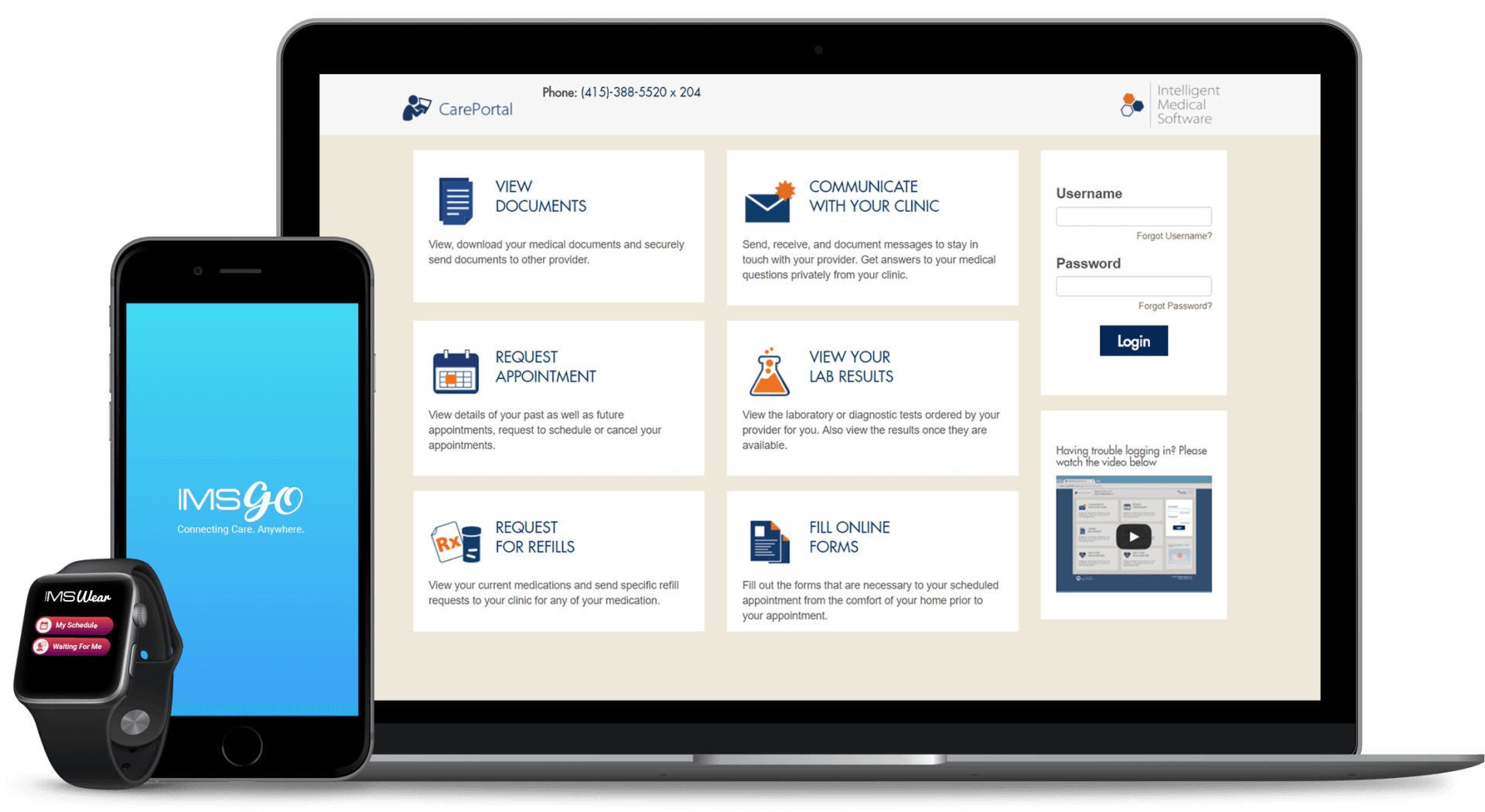
Mobile EHR Apps
As a pioneer in mobile EHR, our solutions have the most advanced cloud and mobile capabilities designed to make healthcare happen anytime, anywhere.
Learn More → -

Medical Billing
Medical Billing / IMS seamlessly integrates the medical billing process directly into your EHR software, meaning increased collections and a faster revenue cycle.
Learn More →
-

EHR
Our EHR system is aligned to meet the demands of a broad and diverse network of healthcare providers.
Learn More → -

EMO
A new branch of modules that expands what IMS delivers for your practice, EMO is the efficiency you’ve always wanted. Whether it’s your front desk, back office, or waiting room, run your medical office like the fine-tuned business it is with our new medical software.
Learn More → -

Practice Management
Our comprehensive practice management tool can boost your medical staff's efficiency, medical billing processes, and patient flow.
Learn More → -

Mobile EHR Apps
As a pioneer in mobile EHR, our solutions have the most advanced cloud and mobile capabilities designed to make healthcare happen anytime, anywhere.
Learn More → -

Medical Billing
Medical Billing / IMS seamlessly integrates the medical billing process directly into your EHR software, meaning increased collections and a faster revenue cycle.
Learn More →
Increase Your Bottom-line
Dr. Tushar Patel, of Children's Medical Centers of Fresno, was able to grow his practice's bottom-line by 28% after implementing IMS.
Increase Your Efficiency
Dr. JoAnn Lin, of McKinney Allergy and Asthma Center, was able to boost the efficiency of her practice's workflow by 80% after implementing IMS.
Increase Your Patient Visits
Dr. Ghassan Safadi, of Safadi and Associates Inc., was able to increase the volume of his patient visits by 30% after implementing IMS.
Increase Your Bottom-line
Dr. Tushar Patel, of Children's Medical Centers of Fresno, was able to grow his practice's bottom-line by 28% after implementing IMS.
Increase Your Efficiency
Dr. JoAnn Lin, of McKinney Allergy and Asthma Center, was able to boost the efficiency of her practice's workflow by 80% after implementing IMS.
Increase Your Patient Visits
Dr. Ghassan Safadi, of Safadi and Associates Inc., was able to increase the volume of his patient visits by 30% after implementing IMS.
One Practice. One EHR Software. One Ecosystem
Your practice can’t fully thrive with an inadequate EHR. That’s why Meditab designed its core EHR software, IMS, to do it all. One of the country’s leading EHR software companies, Meditab empowers practices to succeed with innovative technology and one-of-a-kind flexibility.
So much more than a typical EMR software, IMS integrates every aspect of your practice into one comprehensive ecosystem. Imagine having an EHR with integrated practice management, medical billing, ICD-10 codes, patient engagement, telemedicine features, and more — you can save time and money while improving your practice efficiency. When your EHR does it all, you can elevate your quality of care and ensure a thriving business without the hassle.
Why Our Customers Choose
Meditab EHR Software and IMS

Slide title
Write your caption hereButton
Slide title
Write your caption hereButton
Slide title
Write your caption hereButton
Slide title
Write your caption hereButton

Slide title
Write your caption hereButton
Slide title
Write your caption hereButton
Slide title
Write your caption hereButton
Slide title
Write your caption hereButton
★★★★★
Easy to Use
★★★★★
Functionality
★★★★★
Product Quality
★★★★★
Customer Support
The numbers you need to know:
- 0
- 0
- 0
- 0
Awards & Certifications
We are extremely proud to be an ISO 9001:2015 certified medical software company. This Quality Management Certificate reinforces that our products and services meet the high expectations of our customers.
Meditab is an EMR software company and practice management system. We offer leading multispecialty EHR software solutions designed by providers to meet the unique needs of your practice.
Useful Links
Get the Latest Info, Updates, & Promotions Delivered Directly to Your Inbox!
Meditab | All Rights Reserved.